One thing I’ve noticed that’s pretty universal among women coming in for their yearly well-woman exams is that most of us aren’t entirely sure what a pap screening is, and we’re even more utterly confused by the ever-changing screening guidelines. That’s for good reason. It seems like the guidelines are always changing, and trust me, it gets confusing even to those of us who do this 20 times a day.
However, with the latest and greatest technology available to us nowadays, your doctor is right when he/she says, “Nope, you may not need a yearly pap any longer.” Trust me, it doesn’t mean you’re getting sub-par care, or that your insurance company has decided to be cheap and finagle its way out of paying for something you need and deserve. It’s just that we’ve gotten better at this. We understand it more now. So, sigh. It’s ok. No one is trying to steal your joy of receiving that annual pap that I know you’ve been looking forward to all year long!
 All jokes aside, let me see if I can explain the basics. Maybe this will help next time you see the little Christmas tree bristle brush and speculum emerge from underneath that spaceship table you’re sitting on at the gyn. At least you’ll know it has a purpose…other than just being uncomfortable and unpleasant.
All jokes aside, let me see if I can explain the basics. Maybe this will help next time you see the little Christmas tree bristle brush and speculum emerge from underneath that spaceship table you’re sitting on at the gyn. At least you’ll know it has a purpose…other than just being uncomfortable and unpleasant.
Disclaimer: There is a wealth of information available regarding Pap screenings, cervical cancer, and HPV, and this little segment only scratches the surface. If you have more detailed questions related to you personally, please feel free to schedule a virtual visit with me to discuss in detail. Before you read any further, let me just say that this can definitely be a controversial topic and even somewhat embarrassing. I want to shed light on what the average woman may not know about her body or what the purpose of these exams are. The information provided below is based on sound research and clinical findings from the ASCCP, CDC, American College of Obstetrics and Gynecology, and the National Institute of Health… not my personal opinion. Please also visit their websites for further information and clarity if I manage to utterly confuse you.
What does a pap screening (AKA pap smear) test for?
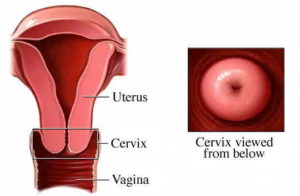
- A pap test is a screening for cervical cancer. The test provides a sampling of cells from the inner and outer portion of your cervix (the bottom of the uterus). A pap can detect cellular changes that are indicative of cervical cancer as well as changes that may suggest that cervical cancer could develop in the future. Let me be clear, paps do NOT test for ovarian cancer, infertility, infection, etc. On occasion, paps may indicate the need for further evaluation for endometrial cancer (cancer of the inside lining of the uterus) or infection. BUT this is not the main purpose of the screening.
Are you 30 or older?
- If the answer if yes, then your pap will now be performed with a co-test that looks at the actual DNA of the cells in the sample. This DNA test is screening for HPV to help determine your risk for developing cervical cancer in the future. I’ll explain more below.
What is HPV?
- Human Papilloma Virus. HPV is a set of over 100+ related viruses, some of which cause warts and others, cancer (cervical, vulvar, vagina, anal, and even oropharyngeal). If you’ve ever had a wart on your finger, you have a strain of the HPV virus. However, there are over 40 strains that affect the genital areas. These are different than those strains that cause your typical aggravating thumb wart.
- We give each strain a number (i.e. HPV 16, HPV 18, etc). These are called the HPV type. Of the 40 types mentioned above, some are what we call high-risk or “oncogenic” strains, meaning that they can potentially cause cancer. The others are considered low-risk strains, and these cause genital warts. High-risk HPV strains are well established as the culprit of nearly all cervical cancer and cervical dysplasia (cellular changes that could result in cancer). The most oncogenic strains that we typically see with cervical cancer are HPV 16 and HPV 18. Other oncogenic strains include types 31, 33, 35, 39, 45, 51, 52, and 58. However, nearly 70% of all cervical cancers are related to types 16 & 18.
- Types 6 & 11 are the two low risk strains that are responsible for 90% of genital warts.
- The HPV co-test that your Ob/Gyn performs with your pap is typically only looking for the high-risk strains.
- Again, a wealth of information exists regarding HPV, but here’s the low down on the basics:
- HPV is a virus that is spread via contact. The types that your Ob/Gyn is concerned with are spread via intimate touch (maybe go look this up if you need a more descriptive description). The kind that your dermatologist is concerned with (i.e. that finger wart) can be spread in a variety of ways including touch, sharing of razers, etc).
- DNA co-testing for HPV only occurs once you reach age 30. Pap screenings begin at age 21 regardless of sexual activity, but we do not screen younger women for HPV. HPV is very common in women younger than age 30. However, most HPV that is found in these women will never cause them health problems and it is not useful to test young women for HPV. Most young women will fight off HPV within a few years.
- HPV is less common in women older than age 30. HPV also is more likely to become problematic for these women, who may have had the virus for many years and their immune systems have not cleared the cells of the virus.
- Pap tests (alone) are still great screening tests for cervical cancer—for any woman ages 21 and older.
- HPV types 16 & 18 are the most oncogenic. If you have a pap with DNA co-testing that comes back HPV positive for types 16 & 18, you will be asked to return for further evaluation.
- Please don’t fret! A positive HPV test DOES NOT mean you have or will ever have cervical cancer. Nearly 80% of women have been exposed to HPV, but nowhere near that number of women develop cancer. Thus, the vital importance of screenings!
How often should I have a pap screening?
- Here is an excerpt from a statement released by the American College of Obstetrics and Gynecology (ACOG):
- “Having a Pap test annually is no longer recommended by leading medical organizations… The guidelines recommend testing every three years for women ages 21-65; routine cervical cancer screening for women under 21 and over 65 is no longer recommended. The two groups also introduced the option of a lengthened, five-year screening interval for women ages 30-65 when screened with a combination of Pap testing and human papillomavirus (HPV) testing.”
- Recap:
- ages 21-30: Pap alone (without HPV co-testing) every 3 years
- ages 30-65: Pap + HPV co-testing every 3-5 years.
- The reason for spacing the time between paps is due to the extremely slow growing rate of cervical cancer and the highly predictive value of HPV testing. If a woman tests HPV positive for the more oncogenic strains, she will absolutely be screened more often for cervical cancer and dysplasia. However, if her pap is HPV negative, there is nearly a 0% likelihood of developing cervical cancer within 5 years.
If I don’t need a pap screening this year, should I still go to my Ob/Gyn for an annual and will it be covered by insurance?
- YES. YES. YES! A pap screening is only a SMALL portion of your annual gynecological exam. The internal exam screens for ovarian and uterine growth abnormalities. The clinical breast exam screens for breast abnormalities. Your provider will also more than likely perform other screenings that should be performed on a YEARLY basis! Annual well-woman visits are usually 100% covered by insurance companies.
- On occasion, your provider may recommend spacing your visits to every 2 years if your insurance provider is Medicare. However, it is necessary that you have a primary care provider perform a yearly clinical breast exam and that you remain up to date on your mammogram during this interval!
What can I do to help prevent cervical cancer?
- A variety of things! Tips from the CDC to prevent acquiring HPV:
- Abstinence
- Mutual monogamy
- Consider the HPV vaccine if under the age of 45
- Utilize protective methods. These are helpful but not entirely preventive.
- Take great care of your body
- If you’ve ever had a pap co-test that came back HPV positive, there are definitely things you can do to build your immune system. A strong immune system is vital and can even help clear the cells of the virus. This does not mean that HPV is cured from your body. It just means that the HPV virus is dormant and should not become problematic.
- Strengthen your immune system by:
- Not smoking; smoking and HPV are the WORST combination
- Getting 7-9 hours of sleep nightly
- Exercising regularly
- Minimizing stress
- Taking a daily multivitamin
- Eating lots of fruits and vegetables
- Taking GREAT care of your BODY
- Strengthen your immune system by:
Can I have a pap while on my period or should I reschedule my appointment?
- You can have a pap while on your period as long as it’s not an extremely heavy day. The newer paps are liquid suspended (not a smear) and allow the blood cells to be spun out of the sample by a really cool machine. So, don’t reschedule or be embarrassed! Your provider is used to it and doesn’t think twice
THAT’s ALL FOLKS! I hope this review was helpful at giving you a better understanding of this extremely complex topic. Again, each case is different, so if you have additional personal questions related to your pap history and overall health, let’s sit down with a cup of coffee in my “virtual office” and talk about it girlfriend! I would LOVE to partner with you when it comes to better understanding your body and how to care for it.



